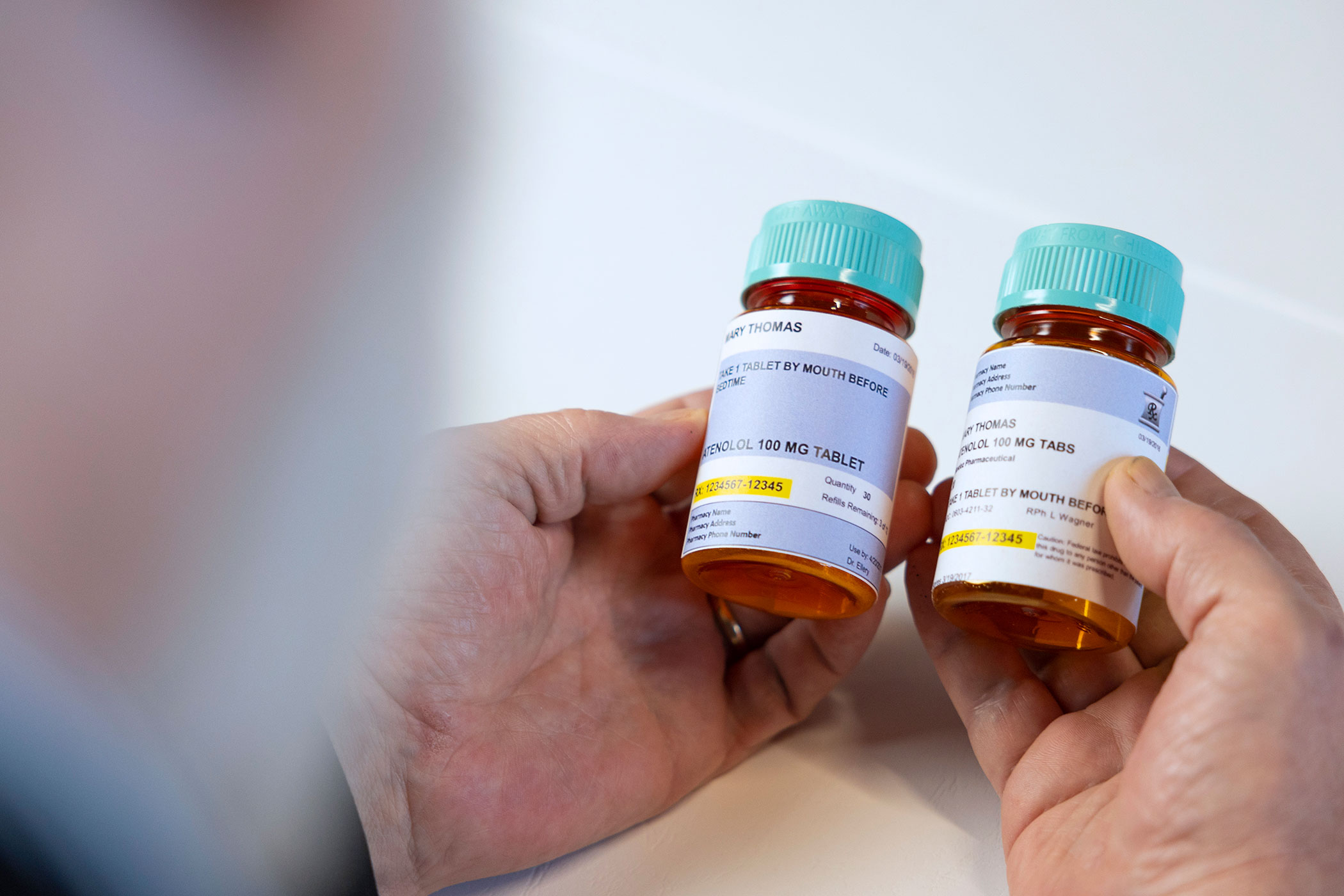
As many as half of all Americans with chronic diseases like hypertension and depression don’t take their medications as prescribed. And more than 100,000 people die due to medication nonadherence each year, costing upward of $100 billion in preventable health care expenses.
But new research from the University of Georgia suggests tweaking the labels on prescription medication bottles could help patients take their drugs the way their doctors intended.
The study found prescription medication labels that list explicit instructions, for example when to take the medicine or whether the patient should avoid alcohol, can dramatically improve medication adherence to antihypertension medications, contraceptives and asthma controllers.

“In order for medications to work, people have to take them,” said Henry Young, lead author of the study and a professor in UGA’s College of Pharmacy.
“Whatever incremental step we can take to positively impact medication adherence is helpful. So we adjusted the medication labels to make them a little bit more friendly for patients. We changed the labels so that patients can pick up their medication bottle and say, ‘Oh, OK. This is how I’m supposed to use this medication.’”
At the beginning of the study, only 65% of patients on contraceptives were regularly taking them as prescribed. With the revised labels, that number jumped to 93%. Participants with asthma experienced a similarly impressive jump, going from only a little over a third taking their medications as instructed to 65%.
Those taking antihypertensive medications also saw an increase from about 80% to more than 90%.
“One key implication of these findings is that improved prescription labels may help patients reach high levels of medication adherence and experience health benefits as a result,” Young said. “People with asthma could see fewer hospitalizations and emergency department visits. Those with hypertension could prevent strokes and congestive heart failure. And individuals using contraception could better protect themselves against unintended pregnancies.”
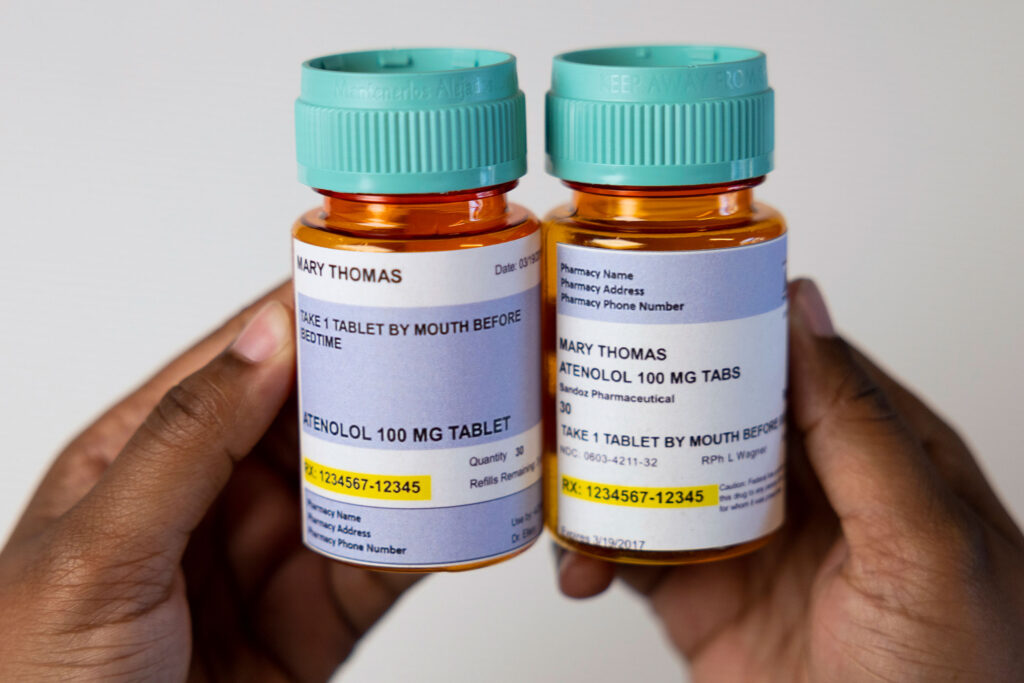
Streamlined labels help patients understand how to take medications
The researchers followed labeling guidelines from the United States Pharmacopeia, a nonprofit centered on patient safety and research, to redesign prescription labels of four categories of medications in multiple pharmacies. The study focused on medications for asthma, hypertension, contraception and depression.
The new prescription labels featured increased font sizes, different background colors in some sections and realigned information to make the information easier to read.
The researchers also moved instructions for how to take a given medication to the top of prescription labels and streamlined the rest to emphasize patient-relevant information, such as “take with food” and “do not drive while taking this medication.” The new labels clearly outlined the quantity of pills in the prescription and the number of refills remaining.
The biggest takeaway is that it is feasible to change medication labels to make them more patient friendly.” —Henry Young, College of Pharmacy
The researchers removed information such as the National Drug Code Directory number and the Rx BIN number, which are used by pharmacies for insurance processing but not particularly relevant to patient care.
More than 1,150 patients at eight different pharmacies participated in the study, filling over 12,550 prescriptions during the study period.
Why don’t people take their medications as prescribed?
A variety of factors lead to medication nonadherence.
Things like high prescription costs, inadequate access to health care professionals and a lack of health literacy all play key parts in people being unable to take their medications as prescribed.
Previous research has shown that health literacy, or the ability to understand and act on health care instructions, is particularly poor in low-income populations. These groups are also at a high risk of a variety of chronic conditions, such as diabetes and hypertension, which require regular treatment with prescription medications. If those patients don’t take their medications as prescribed, their health can decline rapidly.
I would love to see the pharmacy community consider implementing more patient-friendly labels on a larger scale in an effort to help patients take their medications on time.” —Henry Young
All the participants in the present study were enrolled in Medicaid. The researchers chose that group of patients specifically due to their vulnerability to misunderstanding medication labels.
“We addressed that issue by saying, ‘Can we make these labels a little bit more patient friendly? Can we include what the medication is used for? Can we change up the directions so that patients will know how to use the medication a little bit better?’” Young said.
“The biggest takeaway is that it is feasible to change medication labels to make them more patient friendly. But it takes meeting with pharmacists, the folks who create the labels and pharmacy software IT specialists to implement those changes. I wouldn’t say it’s an easy process, but it’s doable.
“I would love to see the pharmacy community consider implementing more patient-friendly labels on a larger scale in an effort to help patients take their medications on time.”
Published in the Journal of the American Pharmacists Association, the study was co-authored by Farah S. Pathan, a doctoral graduate from the College of Pharmacy. The study was conducted with colleagues from Wisconsin Health Literacy, the Medical College of Georgia and the University of Wisconsin-Madison.
The project was funded by Advancing a Healthier Wisconsin endowment at the Medical College of Wisconsin. Additional co-authors include Stan Hudson, David Mott, Paul Smith and Kenneth Schellhase.